Your GP hands you a pathology form with “FBC” written on it. You nod and take it, but you’re not quite sure what it checks or why you need it.
An FBC is a Full Blood Count. It is one of the most common blood tests ordered in Australia. It measures key parts of your blood to help your doctor understand what might be causing your symptoms.
This is not a test that diagnoses anything on its own. Your GP always interprets results alongside your symptoms, health history, and physical exam.
If you are unsure why an FBC blood test was ordered or what it checks, a Online telehealth doctor can explain the test and arrange a pathology referral if needed.
What is an FBC blood test?
A Full Blood Count is a routine pathology test that measures the main components of your blood. It is used to check for signs of anaemia, infection, inflammation, and bleeding or clotting issues.
What it checks:
- Red blood cells and haemoglobin (oxygen carriers)
- White blood cells (immune system cells)
- Platelets (cells involved in clotting)
What it helps detect:
- Anaemia or low iron
- Infection or inflammation
- Immune system problems
- Bleeding or bruising risk
How it is done:
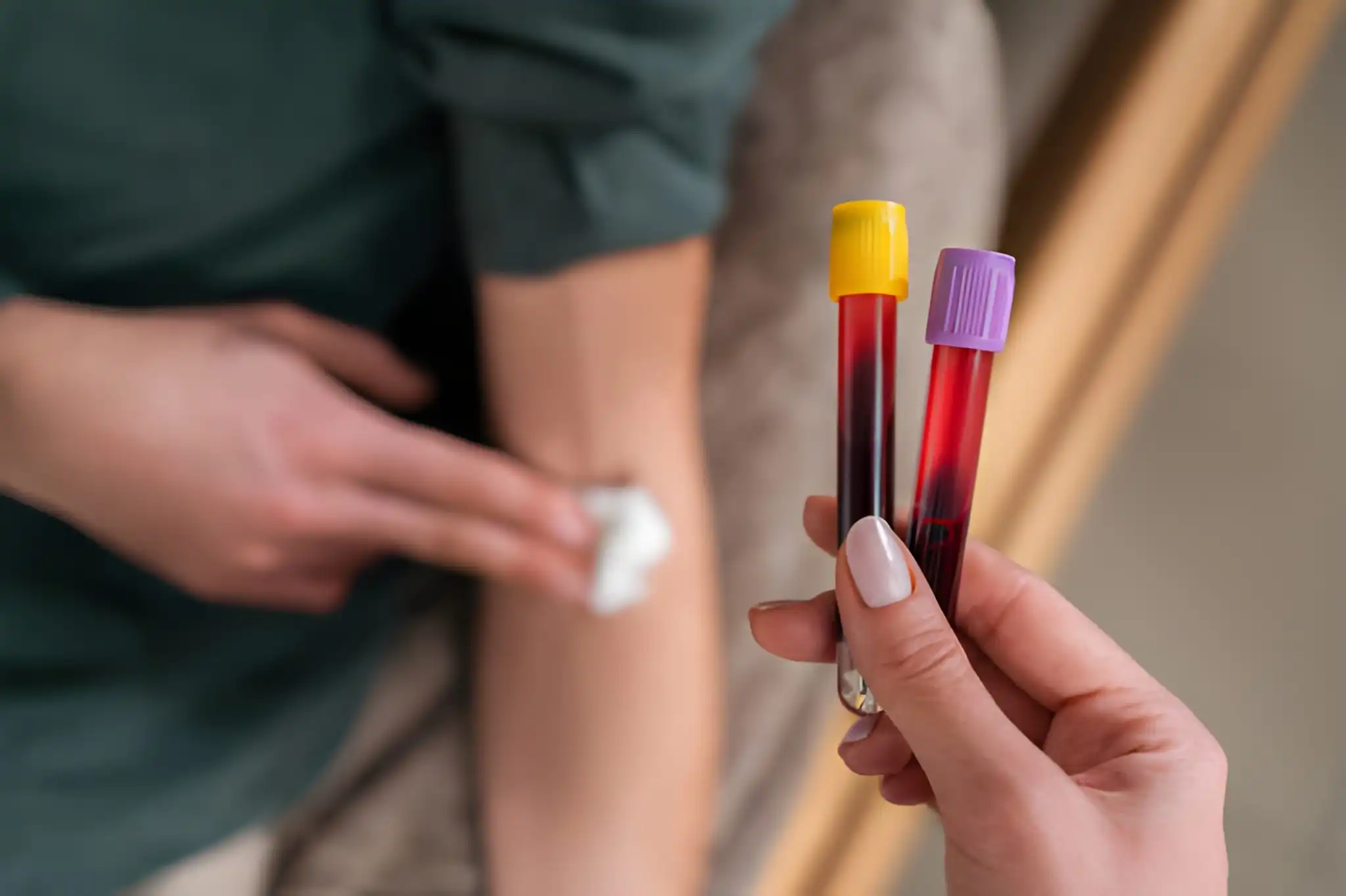
A small blood sample is taken from your arm at a pathology clinic.
How results are used:
Your GP reviews the numbers in the context of your symptoms and health history. One result alone does not give a complete picture.
If you need an FBC blood test for symptoms like fatigue or infection, a telehealth doctor can guide next steps, including repeat testing or additional pathology referrals where appropriate.
What does an FBC check?
An FBC looks at three main parts of your blood. Each part has a different job in keeping you healthy.
Red blood cells and haemoglobin
Red blood cells carry oxygen from your lungs to the rest of your body. Haemoglobin is the protein inside these cells that holds the oxygen.
The FBC measures:
- How many red blood cells do you have
- Your haemoglobin level
- Haematocrit (the percentage of blood made up of red cells)
Low levels may suggest:
- Anaemia
- Iron deficiency
- Vitamin B12 or folate deficiency
- Blood loss
High levels may suggest:
- Dehydration
- Living at a high altitude
- Lung or heart conditions (in some cases)
Your GP will compare your results with your symptoms to decide what it means.
White blood cells
White blood cells fight infection and inflammation. There are different types of white cells, and the FBC counts how many you have in total.
The test may also show a white blood cell differential. This breaks down the types of white cells present.
High white cell count may suggest:
- Bacterial infection
- Viral infection
- Inflammation
- Stress response
- Some medications
Low white cell count may suggest:
- Recovery from a viral illness
- Bone marrow issues
- Some medications or treatments
Your GP will decide if further tests are needed based on your symptoms and the pattern of results.
Platelets
Platelets are small cells that help your blood clot when you are injured. They stop bleeding and help wounds heal.
The FBC measures your platelet count.
Low platelet count may be linked with:
- Easy bruising
- Bleeding that takes longer to stop
- Some viral infections
- Bone marrow disorders
- Certain medications
High platelet count may be linked with:
- Inflammation
- Iron deficiency
- Recent blood loss
- Some bone marrow conditions
Platelet results need clinical review. Your GP will check your symptoms and may repeat the test or order more investigations.
Why would a GP order an FBC in Australia?
An FBC is often part of a routine health check. It can also be ordered when you have symptoms that need investigating.
GPs use it to get a snapshot of your overall health or to look for patterns that explain how you are feeling.
Common reasons include:
- Tiredness or ongoing fatigue
- Dizziness or weakness
- Fever or feeling unwell
- Frequent or prolonged infections
- Checking for anaemia
- Monitoring chronic conditions like autoimmune disease
- Monitoring the effects of certain medications
- Pre-surgery or pre-procedure checks
- Unexplained bruising or bleeding
This test does not confirm a diagnosis. It gives your GP information to guide the next step.
If these symptoms sound familiar, a telehealth doctor can review your concerns and arrange blood tests through a pathology provider when clinically appropriate.
What symptoms can an FBC help investigate?
An FBC is often ordered when you have symptoms that could be linked to your blood or immune system.
These include:
- Persistent fatigue that does not improve with rest
- Frequent infections or slow recovery after illness
- Unexplained bruising or small red spots on the skin
- Pale skin or pale inner eyelids
- Shortness of breath during regular activity
- Dizziness or lightheadedness
- Prolonged bleeding from cuts or nosebleeds
These symptoms can have many causes. Some are simple and easily treated. Others may need further investigation.
Your GP will look at your FBC results alongside your complete medical picture. They may order follow-up tests or refer you to a specialist if needed.
How is an FBC blood test done at a pathology clinic?
The test itself is quick and straightforward. You visit a pathology clinic with your referral form.
Here is what happens:
- Bring your GP referral and Medicare card. The pathology staff will check your details and ask you to confirm your identity.
- A trained collector will take a small blood sample from a vein in your arm. The needle is inserted quickly and removed within seconds.
- You usually do not need to fast for an FBC. Check your referral form to be sure. Some GPs order other tests at the same time that may require fasting.
- The sample is sent to a laboratory for analysis. Results are sent directly to your GP.
- Most pathology services in Australia are bulk billed if you have a valid Medicare card and a GP referral.
Do you need a pathology referral for an FBC blood test? A telehealth appointment allows a GP to assess your situation and issue referrals without an in-clinic visit.
How long does it take to get FBC results?
Turnaround time depends on the pathology provider and your location.
Typical timeframes:
- Routine FBC results: 1 to 2 business days
- Some pathology clinics: same day or next day
- Remote or regional areas: may take longer
- Weekends and public holidays: processing may be delayed
Your GP will contact you once the results are available. Some clinics send results to your MyGov account or a patient portal.
Do not assume that no news means normal results. Always follow up with your GP as planned.
Once your FBC results are available, a telehealth doctor can review them with you and explain what the numbers mean for your health.
Understanding “normal range” on your FBC report
When you look at your blood test report, you will see numbers next to something called a reference range or normal range.
This range shows what is typical for most healthy adults. It does not mean that every number outside this range is abnormal or dangerous.
Your results can be affected by:
- Age and sex
- Pregnancy
- Dehydration
- Recent illness or infection
- Medications
- Altitude (if you live in a high-altitude area)
- Time of day the blood was taken
A single result that sits just outside the normal range may not be a concern. Your GP will interpret it in context.
Do not try to diagnose yourself from one number. Blood test results need clinical review.
Blood test results need a clinical context. If any FBC values concern you, a telehealth appointment can help clarify whether follow-up testing or treatment is needed.
Common FBC result patterns
Specific patterns on an FBC can point your GP toward possible causes of your symptoms.
These are not diagnoses. They are clues that help guide further investigation.
Low haemoglobin:
This is often linked with anaemia. Common causes include iron deficiency, vitamin B12 deficiency, folate deficiency, or blood loss.
Your GP may order iron studies or vitamin level tests to find the cause.
High white blood cell count:
This can appear during infection, inflammation, or physical stress. Sometimes it is a normal response to illness.
Your GP will look at your symptoms and may check inflammatory markers like CRP or ESR.
Low white blood cell count:
This can happen after a viral infection or with certain medications. It may also suggest bone marrow issues in some cases.
Your GP may repeat the test or refer you for further review.
Low platelet count:
This can be linked with easy bruising or a higher bleeding risk. Causes include viral infections, autoimmune conditions, or bone marrow disorders.
Your GP will assess your symptoms and may order a repeat test or specialist referral.
High platelet count:
This can occur with inflammation, iron deficiency, or recent blood loss. It is not always a concern, but it may need monitoring.
Your GP will decide if further investigation is needed based on your complete clinical picture.
What happens if your FBC is abnormal?
An abnormal result does not always mean something serious. It means your GP needs more information.
Common next steps include:
- Repeat FBC to confirm the result
- Iron studies to check iron levels
- Vitamin B12 and folate tests
- Inflammatory markers like CRP or ESR
- Kidney or liver function tests
- Referral to a specialist if needed
Your GP may also review your medications, ask about your diet, or check for signs of infection or bleeding.
Some abnormal results improve on their own. Others may need treatment or monitoring over time.
When you should contact a doctor urgently
Most FBC results are reviewed during a routine follow-up appointment. But some symptoms need urgent medical attention.
Seek emergency care if you experience:
- Chest pain or severe shortness of breath
- Fainting or confusion
- Heavy bleeding or black stools
- Severe weakness that comes on suddenly
- High fever with a stiff neck or rash
Call 000 or go to your nearest emergency department.
For non-urgent concerns about your blood test results, contact your GP or book a telehealth appointment.
Telehealth and FBC tests: what you can do online
Telehealth allows you to speak with an Australian-registered GP from home or work.
What telehealth can support:
- Discussing symptoms that may need an FBC
- Issuing pathology referrals when clinically appropriate
- Reviewing FBC results and explaining what they mean
- Arranging follow-up tests if needed
- Providing advice on next steps
What telehealth cannot replace:
- Physical exams that require in-person assessment
- Emergency care
- Specialist consultations that need hands-on examination
A telehealth appointment allows you to speak with an Australian-registered GP, discuss symptoms, and receive pathology referrals for blood tests when clinically appropriate.
FAQs:
What is a blood test for FBC?
FBC stands for Full Blood Count. It is a standard pathology test that measures red blood cells, white blood cells, and platelets in your blood. It helps GPs investigate symptoms like fatigue, infection, and bruising.
What is an FBC blood test used for?
An FBC is used to check for anaemia, infection, inflammation, and bleeding or clotting issues. It is often ordered as part of routine health checks or to investigate symptoms like tiredness or frequent illness.
Do I need to fast for an FBC blood test?
You usually do not need to fast for an FBC. However, your GP may order other tests at the same time that require fasting. Check your pathology referral form to be sure.
How long does an FBC blood test take?
The blood collection itself takes less than five minutes. You will spend a few extra minutes at the pathology clinic for check-in and paperwork.
How long do FBC results take in Australia?
Most FBC results are available within 1 to 2 business days. Some pathology providers offer same-day or next-day results. Your GP will contact you once the results are ready.
What does low haemoglobin mean on an FBC?
Low haemoglobin usually suggests anaemia. Common causes include iron deficiency, vitamin B12 deficiency, or blood loss. Your GP will order further tests to find the cause and recommend treatment if needed.
Can an FBC show infection?
An FBC can show signs that suggest infection, such as a high white blood cell count. However, it does not identify the type of infection. Your GP may order additional tests to confirm the cause.
Should I worry if my FBC is abnormal?
Not always. An abnormal result means your GP needs more information. Many abnormal results are mild and easily treated. Your GP will explain what the result means and what happens next.
Can I get a blood test referral online in Australia?
Yes. A telehealth GP can assess your symptoms and issue a pathology referral when clinically appropriate. The referral can be sent to a pathology clinic of your choice.
If your question is not covered here, a telehealth doctor can provide personalised advice and arrange blood testing if needed.
Summary
An FBC checks three key parts of your blood:
- Red blood cells and haemoglobin (oxygen carriers)
- White blood cells (immune system)
- Platelets (clotting cells)
It helps investigate symptoms like fatigue, infection, anaemia, and unexplained bruising. The test is done at a pathology clinic with a quick blood sample.
Results are sent to your GP. They will review the numbers alongside your symptoms and health history. Abnormal results do not always mean something serious. Your GP may repeat the test or order follow-up investigations.